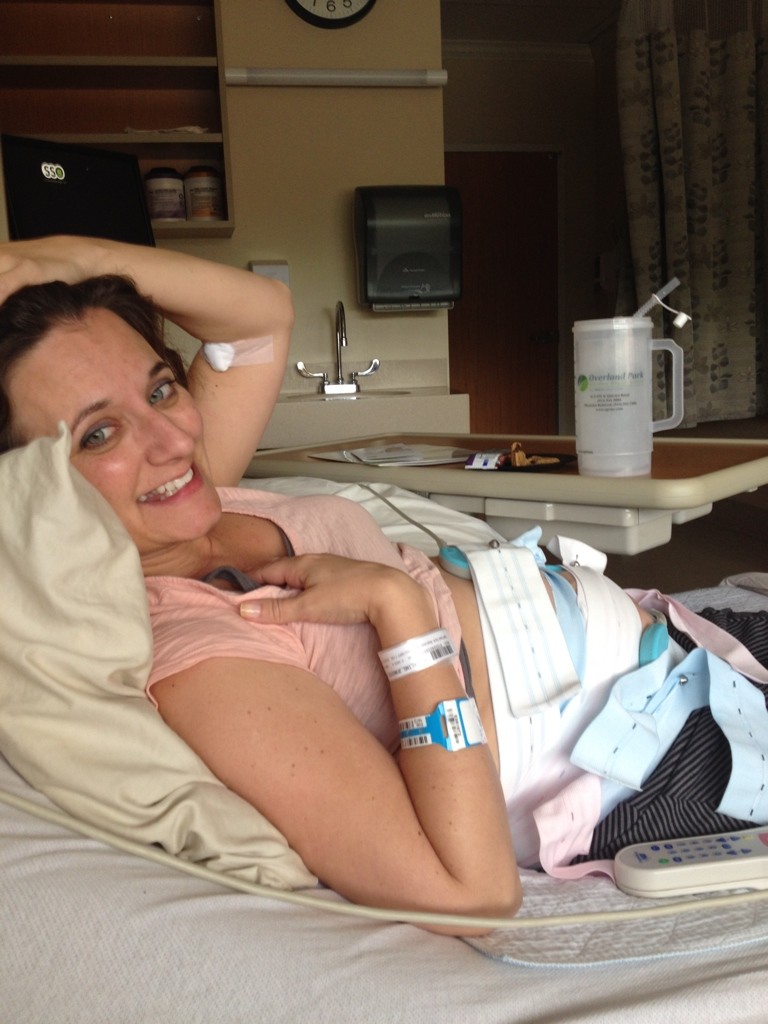
My first week in the antepartum unit was fairly uneventful. I was actually enjoying having all my meals delivered, having daily housekeeping service, and having zero laundry–it was a real mommy vacation! I would walk the halls of the maternity floor, read my stack of books, and binge watch TV. Oh and nap…Ah–the naps! Whenever. I. Wanted. Yep–life in the antepartum unit started out like a retreat… (minus the blood draws).
Momo Twins | Post Series
- A Momo Twins Pregnancy Part 1 – Ignorance is Bliss
- A Momo Twins Pregnancy Part 2 – It Get’s Real
- A Momo Twins Pregnancy Part 3 – Ready or Not, Here Come the Babies!
And the nurses…The nurses were so LOVELY–truly, I think all maternity/labor and delivery nurses have a special spot in heaven–and the girls in the antepartum unit were no exception! These amazing ladies deal with all the highest of the high risk pregnancies…and the hormones, and the stress, and the smell (I know I started to get a little funky once I had to lie perfectly still for 23 hours a day…just laying there sweating with my 40 extra pounds). Bless you, Sweet Nurses!
The Mommy Retreat Takes a Turn
But it wasn’t long before my fetal heart monitoring went from every 3 hours–to just letting me off the monitors long enough to potty and shower. My twins began to show signs of stress.
Our girls were monoamniotic (also called momo or mono mono) twins. This means they were sharing an amniotic fluid sac (apparently, everyone is supposed to have their own)–putting them at very high risk. The umbilical cords of monoamniotic twins become entangled–resulting in a 50% mortality rate for those that are not regularly monitored in the hospital. You can read more about the various types of twins in my Momo Twins Pregnancy: Part One Post (I talk about the shock of finding out I was pregnant with twins–and learning they were momo). Thankfully, I had my entire pregnancy to come to terms with being on hospital bed rest. Once the girls were confirmed monoamniontic, the goal was to get to 23-24 weeks of pregnancy. Once I reached that milestone (viability), I was admitted into my hospital’s antepartum unit and planned to be monitored until week 32-34. I had time to accept, process, and make plans for all this–including the fact I would be having my first c-section (I have four older children–and up to that point, no c-sections) and of course, premature babies.
Coping With an Extended Bed Rest
If you’re finding yourself on bed rest–please give yourself lots of grace. You may not have had time to plan for this extended hospital (or bedroom) stay, and it’s beyond stressful leaving your family and working out all the logistics of running a household. Like I said–I had plenty of time to wrap my mind around this, and I think it helped me to be excited about making it to this milestone. Additionally, I didn’t have to mourn the pregnancy I thought I would have or the delivery I had envisioned. This pregnancy was set apart from the very beginning.
Please know, it is very natural to feel angry, sad, guilty, disappointed, and stressed out–long-term bed rest is a lot to process! But just because you feel something doesn’t make it true–especially, when it comes to guilt! You didn’t do anything wrong–you are a wonderful mom! To combat all this stress and gain some level of peace, my best advice is to choose thankfulness. You are doing the very best thing to keep your baby (or babies) safe. It is hard–but so worth it. And what a blessing to be able to have amazing doctors, nurses, and facilities that make having our miracle babies possible. Another time or another place–this may not be our story. But God placed you and your baby/babies in this time and place–I am forever thankful. In addition to my own troubles–I became acutely aware of horrifying world events that summer (2014). Women and children (and men–but I couldn’t stop thinking about the moms–the pregnant moms, the moms with newborns and toddlers)–they were fleeing terrorists in Iraq…desperately seeking refuge. Can you even imagine? Here I was in my safe, air-conditioned, 3-Meal-A-Day, high-tech hospital…How could I want for anything more? I felt and knew in my heart, I was blessed and beyond fortunate.
Fetal Monitoring
So–anyway…my relaxing hospital stay soon changed from spa-like to mild torture. The babies began showing signs of stress about a week into my hospital stay. The stress was evident in strange heart rate decelerations (and sometimes accelerations). And so the twins earned extra monitoring. Which meant I needed to lie perfectly still for hours—my slightest movements often resulted in losing one of the readings on the twins (they were still so small it was difficult for the nurses to find their heart beats).
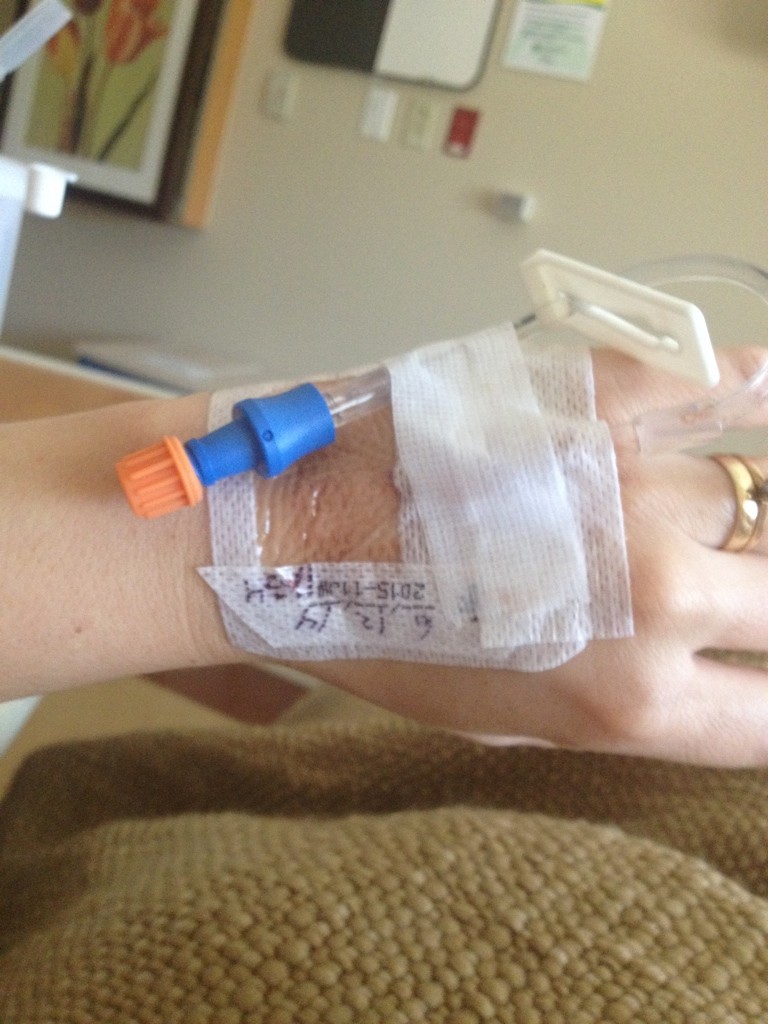
Important Tip About My Personal Nemesis—The IV
Eventually they made me get an IV…which is truly one of my least favorite things in the entire world (and was one of my biggest fears about the hospital stay). Thinking about them raises my stress level ten notches. I just don’t do IVs well…I’ve had enough of them in my 40 years on the planet to know things aren’t going to end pretty. The nurses always think I’m exaggerating or being a baby (and that part I am guilty of). But then they realize—Girl was telling the truth! If you have issues with IVs like me and the nurses are not able to get it done—ask very sweetly for the anesthesiologist to be summoned. They can do a hard stick like it’s nothing…easy peasy (if IVs can ever be described that way). I’ve had many experiences with this—just ask for the anesthesiologist (or someone from their department—their PAs are fantastic too). The nurses will probably still try to do it first—so don’t expect the anesthesiologist to come running for the first attempt…But don’t be afraid to call in the big guns if need be!! You will survive—and you will be glad you have that IV in the event of an emergency…
False Alarm(s)
I think we had about three false alarms—situations where a doctor from my OB office was called. Each time, the doctor came really close to delivering the twins—but then the girls would become stable again and everyone calmed down. My nurses began giving me all the shots necessary to help the babies mature their lungs. My doctors began talking to me about premature babies—and how each day we were able to continue the pregnancy helped the girls exponentially. We reached the 26 week mark, and my doctors were pleased. I was told the next time the twins gave us a scare—it would be the last time…we would be delivering babies.
Processing the Unimaginable
All of this intense monitoring lasted about 2 weeks. When I had first entered the hospital, the NICU doctors visited me and talked to me about different developmental milestones for unborn babies. They went over all the statistics and complications that can occur when babies are born early. But while listening to them, I really wasn’t worried—I truly didn’t think my babies would come extra early. I mean—hello…I had made plans and had the whole summer scheduled out—those babies weren’t coming for 10 more weeks! All my other babies were late—so the concept of early babies just sounded crazy. Yes, they were obviously going to come early—but surely not before 30 weeks…
And then it became evident that the unimaginable was in fact, likely. Oh how I prayed for my girls—and how all my friends and family prayed. And while facing all this unimaginable –I felt peace. I clung tightly to God’s word—this particular verse was powerful to me during this time:
“Your eyes saw my unformed body; all the days ordained for me were written in your book before one of them came to be.” Psalm 139:16 (Truly all of Psalm 139 is perfectly beautiful for expecting moms).
I realized that God already had a plan for my precious daughters—and it was beyond my power and control. I had to acknowledge that God is good—regardless of the outcome. He could be trusted. He loved my girls and knew them perfectly. I had to give their lives to Him completely—and whatever happened, I decided that my heart would praise Him—blessed be the name of the Lord.
“Give Me 4 More Seconds!”
Those were the last words I heard as the anesthesiologist was putting me under…
At 26 Weeks and 4 Days, my beautiful Zoe and Isabelle entered the world!
The morning started off like any other—I had just gotten up to take a break from the monitor (go potty). But then my nurse came in and asked me to hold off on eating my breakfast, which had just arrived. She wanted to get me hooked back up quickly and explained she’d been having trouble monitoring one of the babies. So I got back on the bed, and we proceeded to try and find that little heart beat—but we weren’t having much luck…And so other nurses came in to help. And more nurses began to gather. And the emergency obstetric surgeon from the hospital was called to my room. A mobile ultra-sound machine had been wheeled in…The doctor worked the machine herself—and immediately announced that we were having babies right now.
My precious nurses pushed my bed out of the room and began running it down the hall…They squeezed my hand and said they were praying. The nurses were calm, but intense–the stress and magnitude of the situation was palpable, but they assured me that everything would be okay. One was in charge of calling my husband…I would be having these babies alone.
Once in the surgery room, I remember using every bit of strength to quickly get on the surgery table. I remember people pulling and cutting my clothes off, pouring iodine on my abdomen, and having an oxygen mask placed over my mouth. It was all fast. Very fast—but also didn’t feel fast enough. I knew one of the babies (my Zoe) was struggling.
The chorus to the song, “Forever Reign,” by Hillsong Worship was running through my mind. My soul was crying out to Jesus like never before. (Now I literally cry every time I hear the song.)
And then the surgeon called out, “Are we ready? Can I start?”
To my relief–the anesthesiologist replied, “Give me 4 more seconds!”
Waking Up
The next thing I remember is waking up in a post-op room—my husband discussing my care with the nurse and waiting by my side.
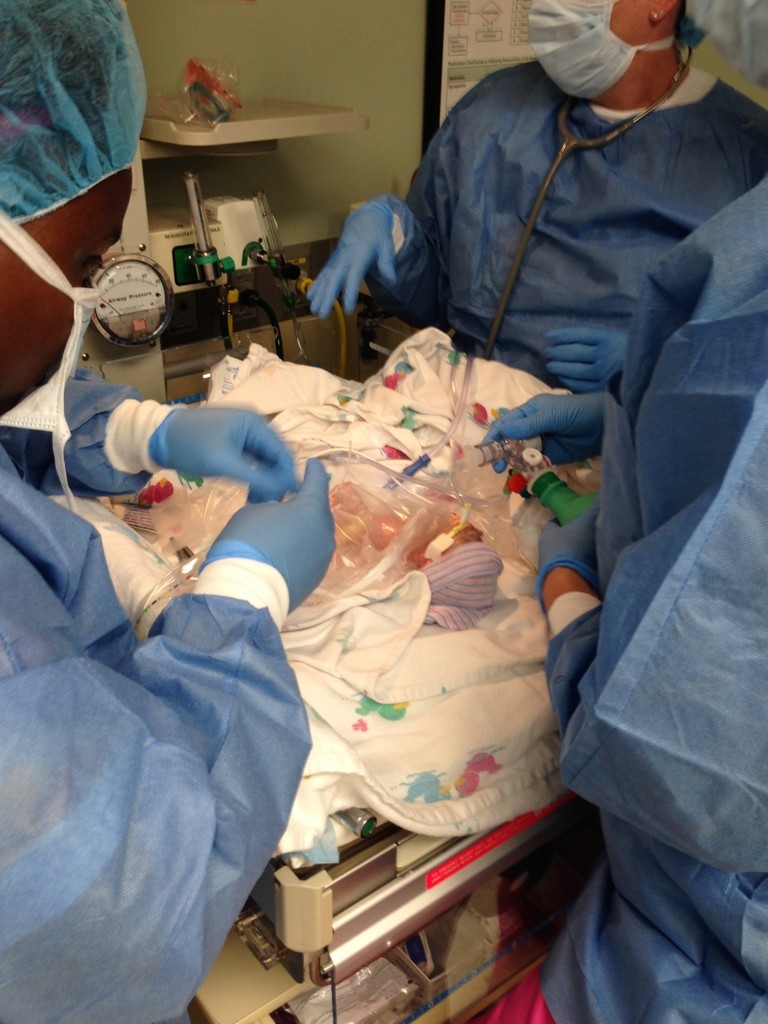
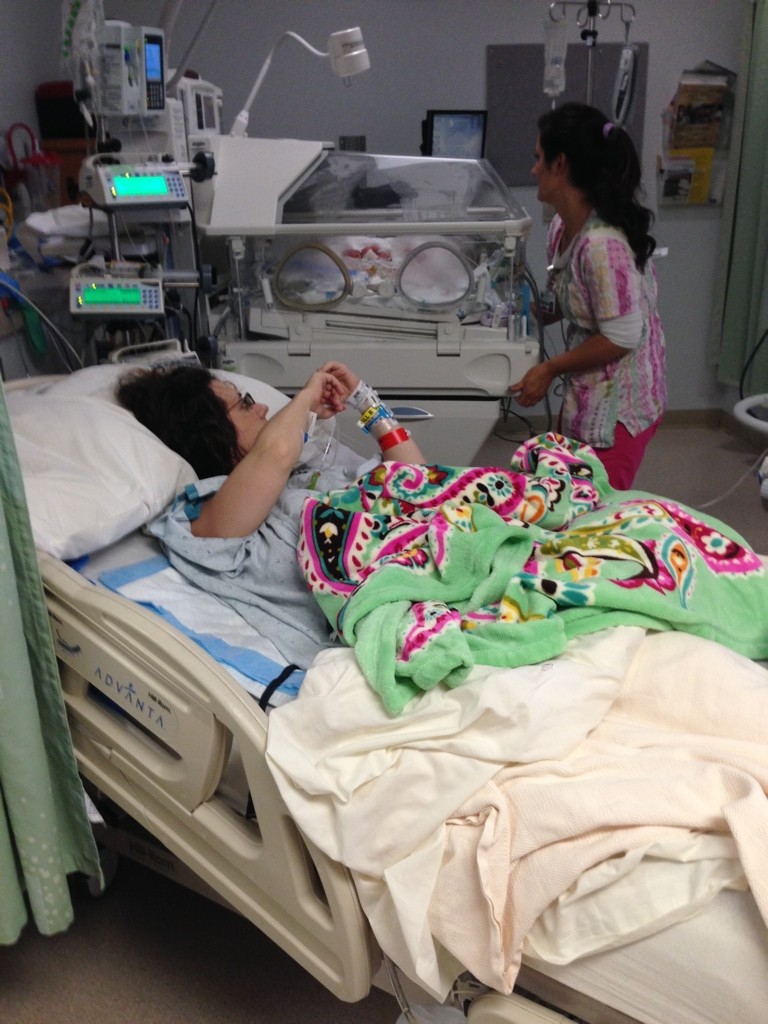
He had missed the births, but was allowed to enter the operating room while the babies were receiving their initial evaluations and treatments (and I was being sewn up). I was incredibly groggy as he explained the current situation–but thrilled to know that both girls were alive and receiving care in the NICU.
NICU
Well the NICU…that is a whole other story. I will share our experience in another post soon (this post has already become a book—thanks for sticking with me)! But for now—please know that the twins are perfectly happy and healthy 3 year-olds! Praising God for them every day!
I hope their story encourages you—especially if you are facing a high risk pregnancy. It isn’t something I would wish upon anyone, nor would I want to live through it again. But I would never want to erase it—it was a painful, beautiful, important part of my life. I am blessed.
With Love,
Jen xo
P.S. If you have any questions about an antepartum hospital stay—please don’t be shy! I’d be happy to help in any way I can!